Healthcare
Nurses needed now: Solutions to a long-running staffing crisis have been hard to come by.
Hospitals and nursing homes hope turnover in Harrisburg means change for the struggling industry.
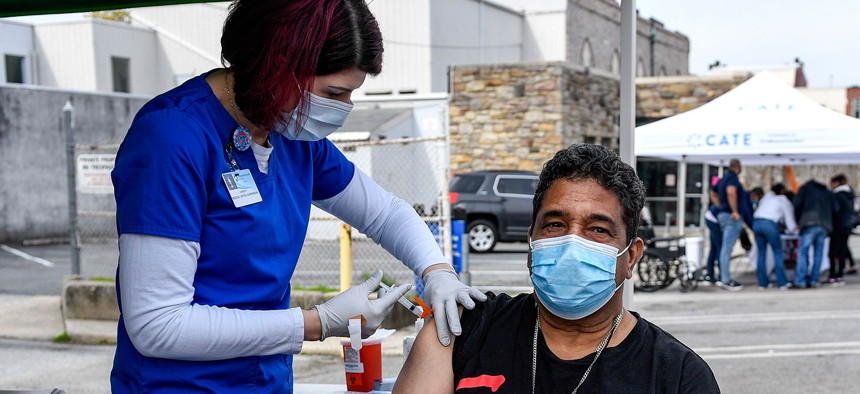
A nurse gives a man a dose of the COVID-19 vaccine during a mobile clinic setup in Reading in April 2021. BEN HASTY/MEDIANEWS GROUP/READING EAGLE VIA GETTY IMAGES
The need for nurses isn’t new. But now, with older nurses opting to retire, new nurses coming in with a COVID-disrupted education, and veteran nurses leaving the industry altogether, staffing shortages are at a dangerous level, as indicated by an American Nurses Foundation survey from last year that found more than 90% of nurses reported staffing shortages at their organizations.
From nursing homes and long-term care facilities to hospitals and even nursing school programs, advocates and lawmakers are grappling with ever-spiraling demands to increase the state’s supply of nurses. And even as Gov. Josh Shapiro included a tax incentive of up to $2,500 for those looking to join the nursing workforce in his inaugural budget proposal, those on the front lines emphasize that dire conditions on the ground warrant more aggressive initiatives to replenish the highly specialized workforce.
“We are hemorrhaging nurses that want to work at the bedside,” Wayne Reich, CEO of the Pennsylvania State Nurses Association, told City & State. He said efforts to recruit new nurses must coincide with improvements in working conditions – or else providers will continue to struggle to retain workers.
“The new generation is coming out of nursing school, they’re spending four years of education, they’re going into debt, and they’re going out and working…They’re saying, ‘This isn’t what I signed up for’ – and they leave the profession.”
Staffing shortages have made it difficult for facilities to maintain low patient-to-nurse ratios, and with increased burnout and an aging population in need of more care, issues surrounding the shortage are compounding the ill effects. Everything from a convoluted regulatory system and an inundated licensing board to a new generation of workers demanding better working conditions has providers scrambling to fill open positions. Beyond short-term measures, advocates are asking for everyone in the industry to take a hard look at the unfair burdens placed on its front-line workers by employers, the pandemic and the economy.
“Anytime that we’re perceived that we’re not caring, or we’re not doing something, we’re just expected to do more and more,” Reich said. “If you drop your kids off at the daycare center and they don’t have the appropriate staff, you wouldn’t let your kid be there. But it’s okay to do it at hospitals.”
Nursing nightmare
The Pennsylvania Health Care Association, a trade group representing for-profit nursing homes, released a report earlier this year highlighting the struggles of nursing facility administrators around the commonwealth. The survey found that more than half of the state’s nursing facilities are limiting or denying admissions due to a lack of staffing. The average facility’s waitlist is about three patients, meaning across the commonwealth’s nearly 700 nursing facilities, there are more than 2,000 patients waiting for care on any given day.
“The question becomes, if they’re not able to come into the nursing home, where do they go? Do they travel dozens – if not hundreds – of miles to find that care? Do they stay in the hospital? Or do they stay at home where it might not be the right level of care?” Zach Shamberg, president of PHCA, asked rhetorically during an interview with City & State.
“We heard from more than a third of our providers that they have 21 or more open positions that they simply cannot fill,” Shamberg added. “In one of the oldest states in terms of our population in the entire country, that is a very alarming and distressing trend.”

The issues go well beyond the long-term care community. Members of PSNA and the Hospital and Healthsystem Association of Pennsylvania said nursing shortages at hospitals have persisted for decades, with the pandemic only exacerbating the issues.
In HAP’s most recent workforce survey, member hospitals reported an average 31% vacancy rate for staff registered nurses providing direct patient care and a 32% vacancy rate for nursing support professionals, such as certified nurse or personal care assistants.
In an attempt to address the staffing crisis, Gov. Josh Shapiro introduced a tax incentive in his inaugural budget proposal to anyone who joins the field. The three-year incentive will give up to $2,500 a year to newly certified nurses in the state. The efforts would apply to those who receive a new certification as well as anyone who moves to the commonwealth with a state-recognized credential, but not nurses already in the field. The administration estimates the tax credits could cost the state nearly $25 million, with about 15,000 people qualifying for the refund.
Those in the industry say it’s a step in the right direction while adding that Shapiro’s budget overall comes up short.
“It doesn’t do anything to address the retention issue. I think that’s a good start, but it needs to be built out,” Shamberg said. “What we were disappointed in with the governor’s budget was that no new funding has been proposed for nursing homes. That would truly handicap this industry in terms of meeting new staffing guidelines not just this year, but next year as well.”
Care at a cost
Providers will continue calls for increased funding, but higher wages and other benefits can only go so far when there are more open positions than there are certified nurses to fill them.
“I often liken it to musical chairs,” said Susie Tack Beardsley, chief administrative officer and a third-generation owner of Quality Life Services nursing facilities in western Pennsylvania. “People are moving from provider to provider, but when the music stops, there are a ton of chairs open.”
Nurses who worked through the pandemic are now seeing colleagues leave and providers struggle to fill the vacancies, putting even more stress on existing nurses who could quickly burn out too.
A former Philadelphia-area nurse who spoke with City & State on the condition of anonymity said the hospital she worked at has dragged its feet when it comes to helping existing staff and filling open positions.
She said the hospital sought to have a 1:5 nurse-to-patient ratio prior to the pandemic, but that shortages were becoming commonplace even before COVID-19 flooded facilities with patients. She added that since the pandemic, staffing needs have only increased while new nurses coming into the field are lacking the clinical expertise missed out on during the height of the pandemic.
“The way that these COVID nurses were trained is just unsafe overall. So you have the new people who graduated jumping in that didn’t really get proper schooling because the whole school was in a hybrid system,” she said, recalling an instance this past summer where she and an inexperienced nurse were overseeing an entire floor of 19 patients.
“I was lucky that I was already a nurse with some experience, but for someone who wasn’t to be put in a position like that, it could have ended up really bad,” she said. “She was asking me questions about her people and I didn’t know any of her patients … On top of dealing with the stress of being way short-staffed, I’m also helping someone else out on the floor. It was too much to handle on my plate because she was being unsafe, and I didn’t feel safe with her.”
An often-cited study from the Journal of the American Medical Association showed that the likelihood of death increases by 7% for each additional patient in a registered nurse’s workload above the recommended 1:4 ratio.

One particularly popular route to fill positions is outsourcing. Hospitals and other providers have used traveling nurse agencies to fill the void, but it comes at a cost.
PHCA’s workforce survey found that 81% of nursing homes in the state are using contracted agency staff to fill open positions. The average hourly wage for a certified nurse aide within a facility is $17.26, but for those working for an outside agency, that number rises to $34.90.
Health care providers are having to compete not only with travel agencies offering nurses twice the pay as an in-house position would but also with other industries offering similar wages for significantly less stressful work.
“We’ve increased (labor costs) by over 30% since COVID, which is great, except so has Walmart, so has Sheetz, so has Wawa, and so has Giant Eagle,” Beardsley told City & State. “We’re competing with a lot of companies where, frankly, the work isn’t as hard.”
The former Philadelphia-area nurse told City & State that her hospital administrators have attempted to provide more support to existing staff, but those efforts have fallen short. For all the gift-based support and appreciation they’re offered, she said, none of it will make the difference that higher wages and better working conditions will.
“Give us safer patient-staff ratios. No more pizza parties,” she said.
Licensing in limbo
With issues on both the supply and demand sides of the nursing pipeline, providers and state officials are looking at solutions to increase the number of individuals entering the field, but also ensure that working conditions lend themselves to retaining more workers in the long run.
Outside of remuneration, nurses and caregiver organizations alike have called on state officials to enroll the state in the Nurse Licensure Compact to allow nurses from other states to practice in the commonwealth without having to obtain additional licenses.
Shapiro told City & State his administration is considering entering the commonwealth in the multi-state agreement but it’s a “long and complex process.”
The organizations see the State Board of Nursing as a bottleneck within the education system. They said that although the education pipeline should be expanded to meet the needs of the industry, at the same time, there are thousands of potential candidates waiting for certification from the state. The board must review each applicant’s degree, background, and other requirements before they can be approved for licensure.
There are about 220,000 registered nurses in the commonwealth, according to labor statistics, with roughly 170,000 of them currently working at the bedside. Some may be out of the workforce or looking for work, while others are waiting weeks or months for their certification to be approved by the State Board of Nursing.
“Over the past two years or so, especially in the spring, when all of your nursing schools are traditionally having their largest graduation, it was taking months to get through that process. And those are delays that shouldn’t be occurring,” Robert Shipp, vice president of population health and clinical affairs for HAP, told City & State.
Both HAP and PSNA recommended nursing board reforms, calling for an improved credentialing system, ideally with a state nursing board equipped with the personnel and resources needed to keep up with the number of nursing graduates filing with the state.
Shapiro said “the criticism is warranted” and he’s working with the board to implement a 30-day mandatory window for applicants.
“If we say it's going to take 30 days and you hit day 31 and we haven't given you an answer, we're going to give you your money back,” Shapiro told City & State. “The idea is to speed up the process and get professionals like nurses out into their fields as quickly as possible.”

HAP has also called for the creation of a Health Care Workforce Council, led by a chief health care talent officer, within the governor’s office. The council, HAP officials say, would help the administration and legislature prioritize health care infrastructure and reduce the red tape that’s holding many new nurses back from joining the workforce.
“You can have dedicated resources to sort of look at (the shortage) and take a deeper dive into it, see where are the real bottlenecks and how can we address them,” Shipp said. “I think there's only upside there.”
Above all else, advocates say, staffing ratios will be key to retaining nursing in the long run. Regardless of the tax credits or monetary incentives designed to attract people into the field, the working conditions nurses have to deal with are a huge indication of the direction of the industry.
“We have to get some of those fundamental changes where a nurse shouldn't be expected to go in and care for eight patients. It puts their license on the line and (allows for) substandard care,” Reich said.
If providers commit to a 1:4 staffing ratio, he said, nurses will begin to see the light at the end of the tunnel.
“We know we can’t go from the horrible conditions we have now to the ideal conditions that we want to propose,” Reich said. “We’re not going to go from one-to-eight to one-to four-overnight. We will want to build that up so people see the light and say, ‘Hey, this is changing.’”
